FREE PRINTABLE
Create Your Personalized Birth Preferences
Receive our fillable birth preference form that you can print and share with your providers.
Add your name and email below to receive the form immediately.
I was so excited to give birth. I hired a midwife group at an out-of-hospital birth center. I took a childbirth class. I learned about hypnosis and I planned to have a positive, calm, beautiful birth experience. To be completely honest, I thought I would open like a beautiful flower and my baby would fall out. Half-joking, of course, but I intended to have a calm, sweet, private birth. What I got couldn’t have been further from that vision.
I want to note something as I tell this story. This birth was almost 9 years ago. I was 27, I was strong-willed, independent (to a fault in many ways), and I had a sense of invincibility that ultimately didn’t serve me in this experience. The story I am about to share is not an easy one to write. It wasn’t an easy one to live through. It’s also extremely common. And it’s the reason I am the person that I am today. I’m grateful for every single moment of it because without this story I wouldn’t be on the path I am on right now, trying to improve our maternal healthcare system, trying to increase our focus on mothers, and trying to change the world so that my story becomes the exception instead of the norm.
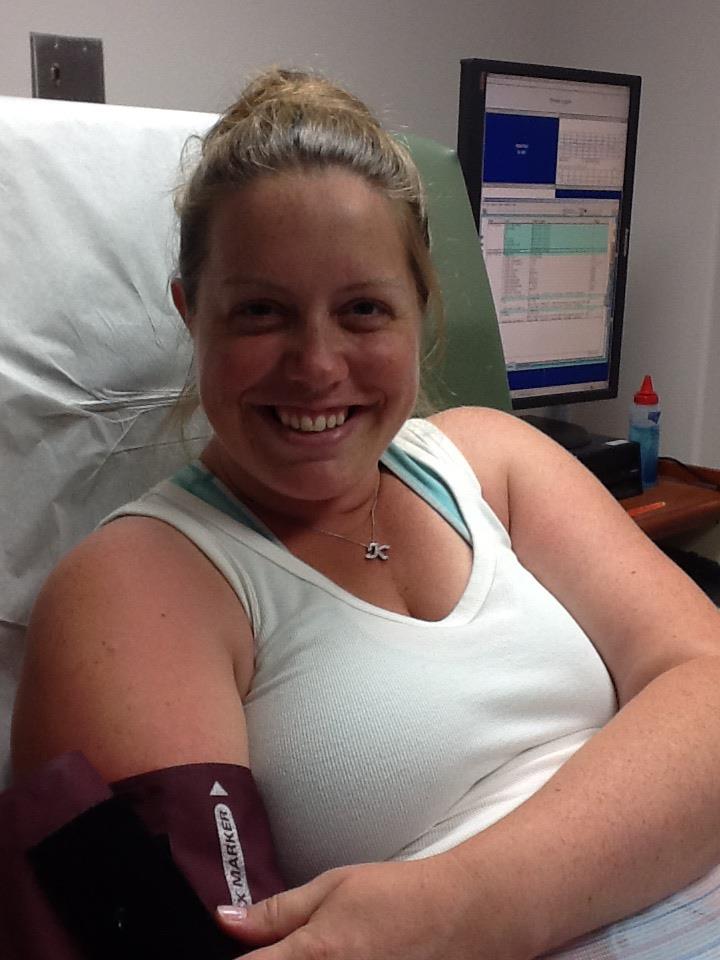
It was July 2012, and we were in the middle of a heat wave. I was 40 weeks and 4 days pregnant and I was at an appointment getting some standard monitoring for that gestation: Sonogram, blood pressure, non-stress test for baby. When the blood pressure cuff deflated I looked at the number on the screen and both of them were over 100. I didn’t know a lot about blood pressure numbers but I was pretty sure that was very high. The tech barely noticed. I had to ask if that was okay. They seemed completely unbothered. The appointment wrapped up and as I was leaving I asked them again about that number. They said they would call my midwife and sent me on my way.
As I walked out of the appointment onto the Brooklyn sidewalk my cell phone rang. The midwife told me I needed to head to the hospital for monitoring, immediately. I hung up and burst into tears. I was alone. It was not going to be the last time I was alone in this journey. I called my husband and my parents and told them I was heading into the hospital and to please meet me there.
One of the midwives, the one who had called me, met me at the hospital. She put me on the blood pressure monitor and had me relax and take deep breaths. My numbers slowly came down. There was a woman who was screaming and clearly either in active labor or pushing her baby out in a room nearby. I couldn’t stop laughing at the noises she was making. Looking back, it must have been a nervous response. I’m the kind of person that laughs at funerals. Sometimes life gets a little too serious and I get the giggles. This was one of those moments. It was fun, funny, and it was all feeling okay. The mood was light.
Before I was discharged to go home and rest something happened. Something that has stayed with me since that day. My midwife told me she was going to examine my cervix. Everyone left the room and when she did the exam it was incredibly painful. I winced and cried out. She said, “If you can’t handle this how are you going to handle labor?” It might seem small to you, reading this now. It seemed small at the time. But it was the first time I questioned if I was in the right care. Why would someone say something so awful and unsupportive while doing such an invasive and painful thing to me? Her words have grown in my memory. Many of the other details of this birth have faded. These words sting still, as a red flag missed, as an attack undefended. This was, in many ways, the foreshadowing of what was to come.
I went home with a 24-hour urine container and was told to return the next day for monitoring. At the sonogram the next day my blood pressure was fine but now my fluid levels were low. Not terribly surprising in retrospect because I hated peeing into a container and basically stopped drinking water, in July, in a heatwave. But I didn’t know that fluid levels changed, that fluid levels aren’t on their own a reason to take any action, that fluid levels can improve with hydration, or that I needed to know any of this to get high quality medical care. I trusted my team. They ultimately didn’t deserve my trust, but I gave it to them.
The same midwife from the day before called, “It’s time to have this baby,” she said. “I just got off the phone with the doctor and he agrees. Head to the hospital for an induction.” And she hung up.
That was it. No discussion. No information. No telling me what to expect or asking me how I felt about any of it. Also, I had never heard of this doctor and had no clue as to why they were weighing in on my care. All pieces of the puzzle I would figure out in the years after this birth. I would learn about how out-of-hospital birth centers in my state weren’t allowed to be owned by midwives. That doctors were calling the shots by design. That I had been misled. That they pulled a bait and switch. That what I was receiving was not midwifery care. But in that moment, I was alone, again, and heading to the hospital.
This is where things get hairy. Instead of being set up in a regular room, I was put in a recovery room. What that means is that rather than being in a private Labor + Delivery room, I was instead put into a shared room, with about 15 different gurneys separated by curtains. There were women who had just come out of their cesareans, in varying states of consciousness, and one nurse named Wendy to care for us all.
My midwife arranged me in the bed, started my induction with oral cytotec (an off-label drug used to stimulate the uterus and ready the cervix for labor), and told me she was leaving. “Call me if anything changes or you need an epidural,” she said. What? Leaving? By this point I was so deep into this experience and so far from where I had envisioned my birth unfolding that I’m not sure I could even fully comprehend that my midwife was leaving me on my own. My one remaining link to the birth I had wanted was walking out the door.
My husband and my mother stayed with me. The cytotec didn’t do anything for the first two doses. So they gave me a third one that was double the previous doses. I had been very comfortable in bed this entire time. Able to talk and eat and excited for what was to come. And then everything changed. Suddenly the contractions that we had been seeing on the monitor started feeling very intense. I got very hot, I writhed in the bed, trying to move and cope with the pain. My mom and husband were like deer in headlights. They didn’t know what to do. I cried out in pain. I wouldn’t let them touch me without cold paper towels on their hands. I asked to get up. I needed to vomit. Wendy, the nurse, would bring me a bin to throw up into and in a way-too-cheery voice tell me that I was dilating and everything I was feeling was normal and good. It didn’t feel good. I felt like a trapped animal.
Wendy wouldn’t let me lay in any position except flat on my back. The monitors would shift and she wouldn’t be able to see the baby’s heart rate and the contractions when I moved to cope with the surges. I asked to go to the bathroom and she looked at me and said, “You are in too much pain, that’s not safe,” as she handed me a bedpan. Technically, I wasn’t chained to the bed, but I might as well have been. I had a blood pressure cuff on my arm, a pulse-ox monitor strapped to my finger, two monitors strapped to my belly, and two pressure cuffs around my legs to prevent blood clots. There were 6 different straps and wires limiting my movement and keeping me in the bed. It was claustrophobic and anxiety-inducing. My every-3-minute cytotec contractions left very little time to figure out what to do about the situation I was in. I wanted to yell, I wanted to rip everything off of me, I wanted to scream. I did scream. I cursed a lot. I hoped that I wasn’t disturbing the half-conscious women nearby.
Typing out these sentences is cringe-worthy. As a doula who has worked with women for over 6 years, teaching them to advocate for themselves, I have a hard time not feeling shame at my inaction. At my silence. At my allowing myself to be silenced. At my sheepishness in letting Wendy make the entire experience about her ability to see the contractions and not about my ability to cope with them. And yet it is in this moment, in telling this story, that I gently remind myself that I needed to be this woman in order to grow, in order to see the problem, and to be set on my life’s path to change these norms and systems that discard and dismiss women during their most challenging times. That I should have been able to walk into my birth and expect that my midwife and medical team would care for me. That I wouldn’t have to hire a person to protect me from the staff at the hospital.
My husband knew my wishes. He knew I wanted to go without the epidural, he knew I wanted a different kind of a birth than what I was getting. I looked at him dead in the eyes and said, “I want an epidural.” I saw him start to protest, I saw him think it was his job to support my previous wishes. I didn’t have time between contractions to explain how everything I had wanted was out the window. How I was trapped in a bed in a torture chamber with a nurse that had a falsely cheery voice, and how I needed help. I said, “This isn’t anything like how I imagined it would be. I want the epidural.” And he listened. Thank god he listened. He didn’t fight me, he didn’t try to convince me, he listened to me and it was one of the few times in the entire experience that someone did. In that moment I needed to be acknowledged. I needed to have some power over the situation.
When we told Wendy that I wanted the epidural she said the strangest thing, “Are you sure? You’ll need to go to an L+D room for that.” I couldn’t process that in the moment. Honestly, almost 9 years later I still can’t. Why would getting a private room be a bad thing? Was an L+D room one of my options this entire time? If that was an option why was I in the recovery room with all these moaning women? Why had my now-absent midwife okayed this? I would have asked for an epidural from the get-go if I knew that was my ticket into my own room! One of the many perplexing moments during this birth.
Before I went I was checked by some doctors (as my midwife had long abandoned me at the hospital). I was 4-5 centimeters dilated. The numbers meant nothing to me, but I’m guessing in retrospect that my progress is the only thing that got me out of the recovery room and fast-tracked me for an epidural. When I got to the room I went to the bathroom and sat on the toilet. I had my husband there with me and I remember wiping and seeing a lot of mucus and a little blood. The contractions that had me screaming while laying flat in the bed were still very intense on the toilet, but somehow they felt manageable. I had a flash of regret, a moment of thinking maybe I wouldn’t get the epidural. But it was just a flash. The new nurse assigned to me demanded I get into the bed. She was not nice. Not warm. Almost angry at my very presence. I listened, I had no fight in me.
Believe it or not, the epidural was the thing I was the most concerned about as I prepped for my birth. The idea of a needle going into my back was almost too much to bear. And even though this is a cesarean birth story, I can unequivocally say that getting the epidural was the worst part of the entire ordeal. The anesthesiologist had everything set up. My husband and mom left the room. The midwife had appeared, apparently someone had called to let her know I was getting pain relief, and she talked me through my contractions as the doctor inserted the needle behind me. I felt the needle. I felt it puncturing my spine. I jumped and screamed. “Are you feeling pain or pressure?” the doctor asked me, sounding more annoyed than concerned. “It’s pain!” I replied loudly. She didn’t care. She kept going. I wasn’t a person at that point. I was a back that needed a needle and my human emotions and reactions were getting in her way. Add her to the list of dismissive, horrible caregivers that I came across throughout this birth.
Once the epidural was in and I had relief from the experience I closed my eyes and rested. Everyone was still in the room. It was the middle of the night at this point. The contractions had kicked in around 11pm and now it was after 3 in the morning. I was exhausted. But every time I opened my eyes, the room was still full of people. The bright lights were on, the nurses, the midwife, and my husband and mother all had very serious faces. The medical team flipped me to my left side. I didn’t question it, I just rested and let them do their work, expecting everything to settle down and for me to be able to sleep for a while.
And yet they all lingered. And their expressions grew more concerned. No one was looking at me. They were all looking at the monitors. The midwife finally clued me in. The baby’s heart rate was racing and then dropping. There was a problem. He was going up to the 190’s and then dropping down to the 100’s. He was in distress. “I’m going to call the doctor and see if they can come in and take a look,” she said, pulling out her cell phone. Once again, at a critical moment this mysterious doctor was calling the shots for me and my baby on the other end of a cell phone. I didn’t want to wait for a doctor. I wanted my baby to not be in distress. I had sacrificed everything that I had wanted for my birth at this point to keep the baby healthy and I wasn’t about to end up not getting that. In one of the only other moments of this entire experience that I was listened to, I looked right at my midwife and said, “I want a healthy baby.” She called the cesarean on the spot and we started prepping for surgery.
I want to make something clear. I do not think that all that matters in a birth is a healthy baby. I know that a healthy baby is one that has a healthy, whole, stable, supported mother. When I asked for a healthy baby it was a request to at the very least, please leave the hospital with a healthy baby. Because everything else I had valued about my birth experience was out the window already. It was a reminder to the midwife that she needed to at the very least protect my baby more than she had protected me.
I was rolled on a gurney into the OR, alone again. My husband would join me when the surgery began. It was cold and sterile with a huge, round, bright light on the ceiling. I remember thinking that this is what I would expect the ceiling of an OR to look like. Everyone did their work. My arms were strapped down to boards and I formed a T shape with them outstretched. I was shaking uncontrollably for much of the night and I begged the doctor to let my arms go because they were aching from the spasms. I was ignored. Strapped down like an animal. Treated as less than human. The doctor told me I would feel some pressure as the baby was taken out. I didn’t feel a thing. I was so incredibly numb. I didn’t mind one bit.
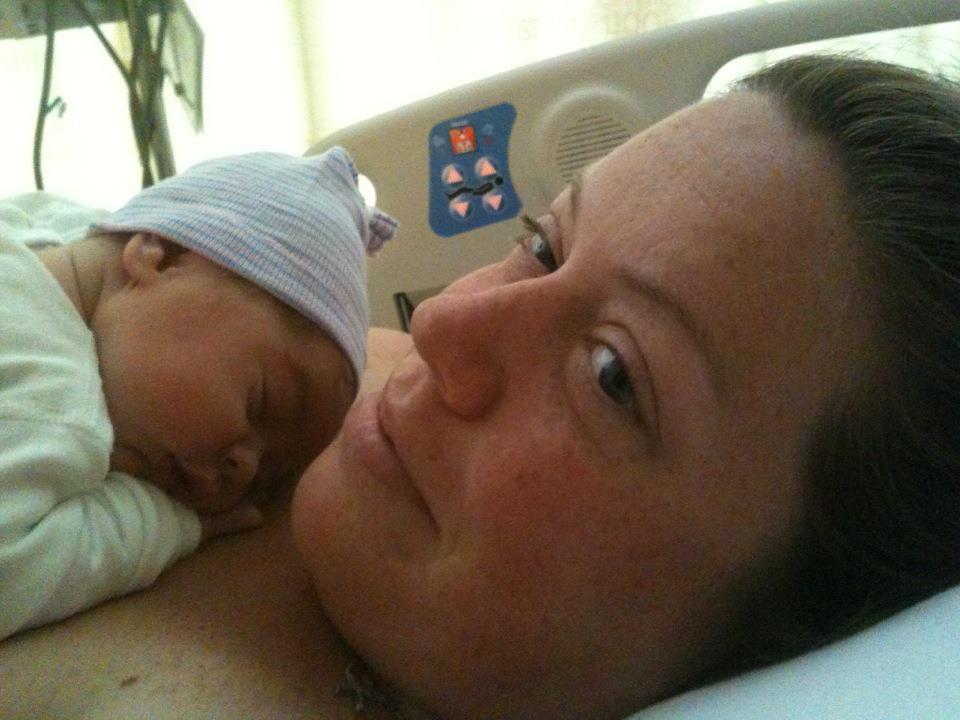
My son was born at 5:20am on July 7th, 2012. He was healthy. I got to kiss his little face and then my husband held him while they sewed me back up. I continued asking for my arms to be unstrapped and instead of listening to me, the anesthesiologist put some medication in my IV that made me fall asleep. My husband asked if everything was okay, as he watched me lose consciousness. The doctor told him I was fine and he had just given some anti-anxiety medication. With no discussion. Instead of unstrapping my arms, he used the only tool he had been trained to use: Medication. Apparently, no one had trained him in consent and patient communication.
We all went back to the recovery room, and Wendy was still there. I was crying with joy, so excited about my baby. She said that most women who are rolled back to this room aren’t joyful. She was so happy for me. My midwife helped me breastfeed my baby. I was so excited to have him in my arms. It all felt surreal. I was in a state of bliss and shock. The trauma I had been through was not fully realized yet. The hormones my body released after birth were making the entire experience fuzzy. I was bonding with my baby, I was in love, I was so joyful.
It wasn’t until I started to prepare for my second birth that I started to unpack what happened at my first. I ordered all of my hospital records. I poured over them, looking for answers. I have reread them after each of my births, and periodically throughout my doula career. And each time I learn something new, I have a new perspective. My healing from this birth experience is ongoing. The more I use the things I learned from this birth to change the system, to make sure other women don’t endure what I endured, the more powerful this experience becomes.
It’s this birth experience that rocked my world, that opened my eyes to the ways we are failing women, to the ways that the system is set up to dehumanize women and decenter them in their care. It was traumatizing, and difficult. But without this birth I wouldn’t have been set on the path I am on right now. I wouldn’t have understood how a strong-willed, loud-mouthed, invincible, independent 27 year old woman could be silenced, dismissed, and stripped of her power. And I wouldn’t have been spurred into a lifelong journey to help women find their power, exercise their right to make decisions for themselves, and to have a motherhood experience that is supported and joyful.
Kaitlin is a mother of three, a doula, and a passionate advocate for access to care during all stages of motherhood. After a traumatic first birth and a transformative VBAC in 2014 she trained with DONA International and began her doula practice. After having her last baby at home in 2016 she co-founded True Birth, a doula team serving families across Long Island, NY. She served on the council of the Long Island Doula Association from 2017-2019 and in 2019 founded Be Her Village, an online gift registry connecting new parents with support services and creating access to funds to pay for this vital support. When she is not working to improve motherhood Kaitlin loves playing chess, cooking, and hiking.

Add your name and email below to receive the form immediately.

